Under-diagnosis of Bronchiectasis Hinders Treatment
Read More
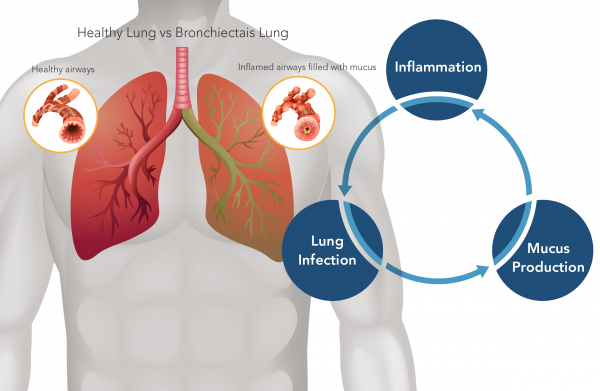
Lung damage caused by bronchiectasis often worsens over the course of the disease. After the initial trigger and during subsequent infections, increased inflammation in the lungs makes it difficult for patients to clear mucus secretions. Mucus buildup encourages the development of additional infections, thereby continuing the cycle of damage.
Airway clearance therapy (ACT) techniques can help thin, mobilize and remove mucus from the lungs to reduce complications from repeated infections and minimize the problems associated with inflammation. Physicians have many therapy options to offer to bronchiectasis patients requiring regular airway clearance.
By making mucus easier to clear, airway clearance therapy allows patients to expectorate lung secretions before the fluids become infected and begin causing more lung damage. A lower occurrence of infections means fewer days spent feeling unwell or being too sick to participate in normal activities. Reducing mucus in the lungs has also been associated with fewer bronchiectasis exacerbations, thus allowing patients to live free from symptoms or with fewer symptoms from day to day.
Airway clearance can improve lung function, making it easier for patients to breathe. Many undergoing such therapies report better quality of life, and since techniques can be tailored to patients’ needs and are suitable for both children and the elderly, ACT shows promise as part of a bronchiectasis treatment protocol regardless of a patient’s age, lifestyle or disease stage.
Overall, the use of airway clearance is a safe way to treat and manage bronchiectasis in most patients by improving expectoration, lung function measurements and the ability to enjoy life. Other therapies, including medications or alternative remedies intended to reduce lung inflammation, may be used in conjunction with ACT as part of a robust treatment protocol. In all cases, the goal of ACT should be to minimize both exacerbations and shortness of breath, conserve energy, reduce pelvic floor stress and improve quality of life. Individual needs dictate which ACT method is best and whether techniques should be combined for a more comprehensive and effective treatment plan.
Typical ACT Techniques include:
Evaluating a patient’s needs to determine the proper protocol for ACT is a vital part of bronchiectasis treatment. High frequency chest wall oscilation, chest physical therapy and other techniques work to clear away mucus, thus minimizing the occurrence of infections and exacerbations. Because many studies and reviews suggest ACT is useful and appropriate for patients of all ages, these techniques are important to consider adding to any bronchiectasis treatment plan.
Several studies and reviews suggest HFCWO is a beneficial technique for patients requiring regular airway clearance. This type of therapy is used to treat many different types of lung diseases in which mucus buildup is a concern, including bronchiectasis. Potential benefits can include:
Experiencing one or more of these positive effects has the potential to greatly improve a patient’s quality of life. One study suggested HFCWO may offer greater benefits than CPT, although no long-term research on the technique is available to determine if this remains true over a prolonged period of treatment.
HFCWO is typically performed using a percussion vest. Traditional models rely on the combination of air bladders, a compressor and a vest worn by the patient, a restrictive setup requiring a visit to a medical facility or complex in-home devices for treatment to be performed. However, new technology is making portable models possible. The AffloVest is one such chest wall oscillation vest built to run on battery power allowing patients to be mobile during use and giving them the flexibility to choose from various levels of intensity for the delivery of customized airway clearance treatment.
The AffloVest gives patients an accessible, portable way to perform daily HFCWO therapy sessions which may have positive effects on their respiratory health and potentially reduce the recurrence of chest infections. Battery-powered and easy to use, this HFCWO vest can be a beneficial part of treatment protocols and may be used in combination with other types of ACT for maximum effectiveness.
Doctors discussing the possibility of ACT with bronchiectasis patients must take the time to thoroughly evaluate individual health histories to determine the best technique or combination of techniques. Several factors are important to consider before making a decision:
A combination of therapy types in addition to ACT is often the best solution for sufferers of bronchiectasis. Physicians and therapists must work with patients throughout the course of treatment to ensure compliance and perform routine follow-up evaluations for efficacy. By looking at the frequency and severity of symptoms, infections and exacerbations, members of the treatment team can determine if and when patients require additional treatments or changes in protocol.
Call us at 1.833.382.2845